Rebuild Your Pharmaceutical Path as a Patient
For most individuals, the prescriber-patient relationship ends when the prescriber rips off a paper with the patient’s written prescription. As a patient, the moment you see the bottom of your prescription bottle, you know it’s time to take a trip down to the pharmacy to restock the pills. Weeks, months, and even years have passed by and you’re in a cycle of refilling your prescription, with poor communication between you and your prescriber. You may not feel the necessity to call up your prescriber because you feel fine, right? If you don’t experience life-threatening side effects, you must think you’re doing ok.
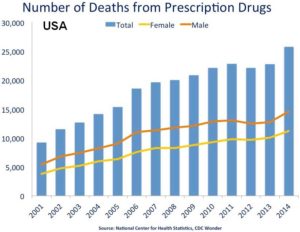
However, patients can still experience minor impairments in their daily activities that they do not notice or think to mention, which can cause severe health risks in the long-run. In the last 5 years, inappropriate use of pharmaceuticals has dramatically increased. And often, the misuse of prescription drugs tracks back to lack of communication between a patient and prescriber. What are some ways can we prevent prescription misuse, leading to health problems and even death?
Look beyond the prescriber
In an interview with Michelle Gross, Managing Director of Spectrum Science Communications New York Office, I asked for her opinion on whether or not she believes prescribers provide their patients sufficient warning about hazardous interactions between their prescription and OTC medicines or drug and alcohol use. “Patients don’t get enough information about the medicine they are taking and the conditions they have…they need to look beyond the prescriber for ways they could get that information” says Michelle, referring to the fact that prescribers don’t have the time to inform every single one of their patients about the details of each prescription.
Michelle suggested the solution may lie in the prescriber’s care team, like a nurse or a physician’s assistant. Patients could use them as the primary point-of-contact when they have a question about their prescription. Maintaining contact once and a while with a healthcare professional could enhance their knowledge about the drugs they take and provide the opportunity to learn how to prevent misuse.
A potential website portal or app
We use smartphones to connect ourselves with our loved-ones through social media platforms, emailing, and instant messaging. Smartphones and mobile devices have become so deeply ingrained in our social lives, it is hard to imagine what we would do without them.
Michelle asked, “Is there an online google-type resource that could be created where patients could check to get an alert every time their medicine changes? We have the technology to do that, there’s no reason why something like that couldn’t be created.” It doesn’t seem realistic for a physician to be responsible to hold every single one of their patient’s hand and guide them towards their medication process. If a website portal or an app was created for patients to track their prescription, it could potentially decrease prescription misuse and fit seamlessly into their daily routine.
Inform to enhance
Patients and prescribers are busy with their own lives. Neither have time to constantly look out for their
prescriptions or remind one another about important information. However, there is a burden of responsibility on the prescribers, as they are the experts, to properly inform the patient of both the benefits and the risks of taking a drug; this description has to be comprehensive, prescription misuse happens (more often) when patients don’t have the information they need. Michelle suggests this burden also extends to patients to be open about their personal lives and to update their prescriber on how a particular medication regime is affecting them. Their past challenges, like a drug or alcohol problems, or a family history of adverse reactions to some medications is crucial information for the prescriber when explaining to the patient the benefits and risk factors of a prescription.
Repair our habits
Imagine waking up one morning to a notification from a drug tracker app on your phone informing you that Tylenol can give you severe adverse reactions when taken with your prescribed ADD medicine. You would immediately avoid Tylenol and find an alternate OTC pain reliever to take. The amount of lives saved would significantly increase if we had the tool to be notified each time our prescription is modified. Prescribers can be more active in encouraging their patients to be responsible and informed about the status and risks of their prescriptions. To prevent incidents of prescription drug misuse, as patients, we must do our parts to responsibly monitor our health while taking prescription medicine and keep our doctors in the loop. By building stronger relationships with our prescribers, we can repair habits of poor communication with one another and properly provide important information about the prescribed medicine and, slowly, but surely, begin to see less prescription misuse.
About the Author:
Fabiana Cuellar is a Public Relations Intern at GLOBALHealthPR
